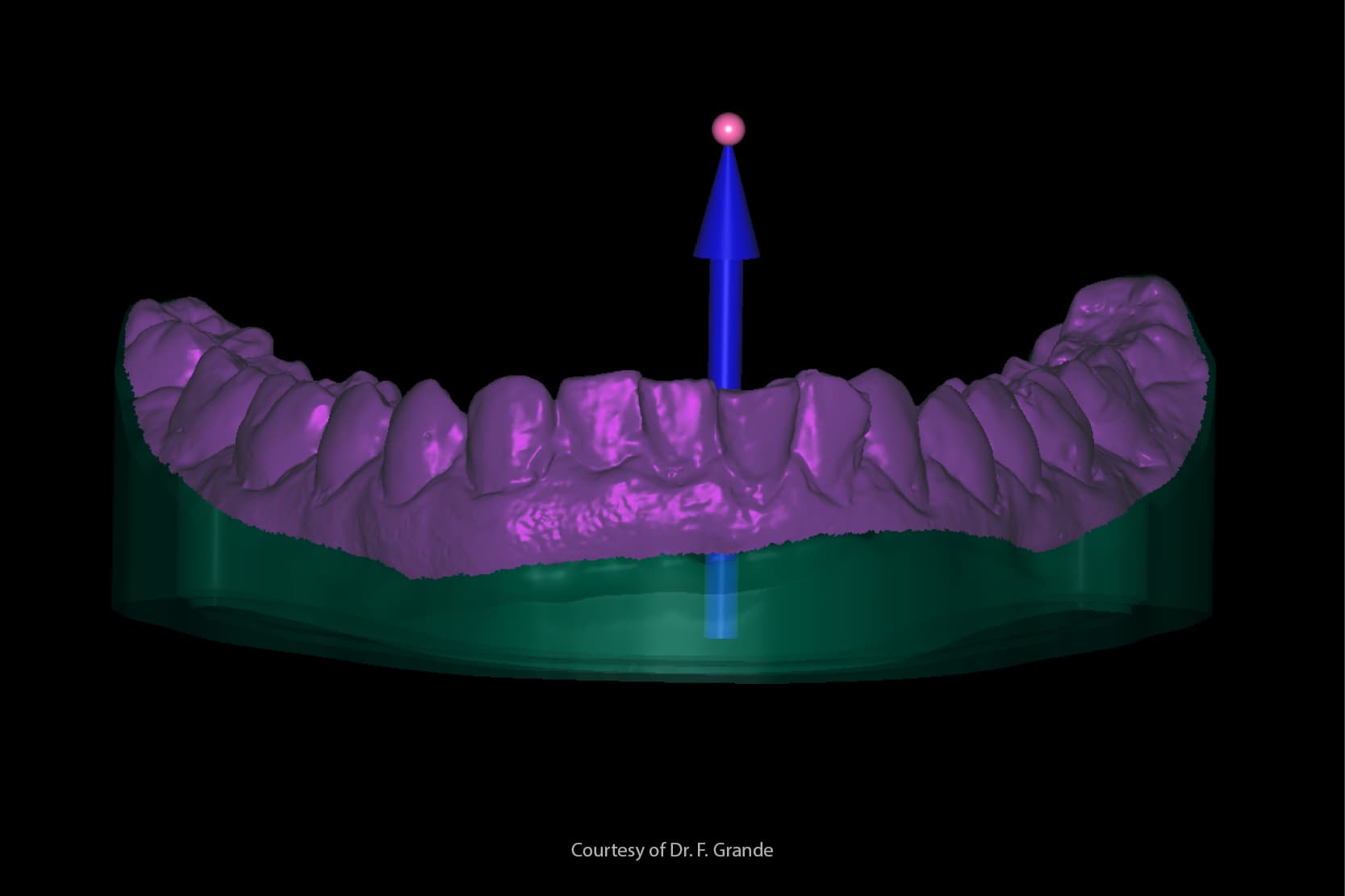
Over the last decade, the spread of Computer Aided Design and Computer Aided Manufacturing (CAD/CAM) has led to the development of digital technologies and new workflows in the field of dentistry. [1] Dentists are making an increasing use of intraoral scanners, which produce STL files and generate three-dimensional (3D) images of scanned objects, to obtain digital impressions of dental arches. [2,3]
Digital impressions offer well-known advantages and also avoid many of the limitations intrinsic to analogue workflows [4]:
- they do not require the casting of stone models;
- they allow models to be evaluated immediately in positive form;
- they eliminate the risk of cross-infection between dental practice and dental laboratory;
- they do not require physical storage space;
- they improve comfort for the patient.
Nevertheless, in certain clinical cases, such as those involving completely or partly edentulous patients, [5] and complete arch rehabilitations on natural teeth or implants, [6,7] conventional impression materials still provide more reliable results.
The digitalisation of dental procedures
The digitalisation of dental practice and laboratory procedures is still very costly and has a relatively steep learning curve. Learning to use the technologies and instruments involved requires a significant effort, especially for older dentists. [8]
It is nevertheless undeniable that digital workflows offer many advantages in time and quality for the dental laboratory. In this context, the use of impression materials made scannable by specific industrial processes may maintain the benefits of conventional materials while simultaneously avoiding the need to produce stone models, a process that can easily introduce errors, leading to longer times and increased costs for the dental lab. [9]
Though materials of this kind are not yet widely utilised, many dentists and lab technicians could benefit from their use and even improve the accuracy of their digital impressions in certain clinical cases. [10]
Scanning implant impressions
The elimination of stone models permitted by the use of scannable impression materials could prove especially advantageous with prosthetic implants, since analogue impression abutments can move as a result of expansion in the stone, leading to complications with the prostheses. [11]
The results of research
One study demonstrates that scans of implant impressions are more accurate than those taken of stone models made from pick-up or conventional impressions. [12] García-Martínez et al.[13] affirm that scannable impressions made from vinyl siloxanether can be digitalised with greater overall accuracy than those made from conventional elastomer materials.
However, other studies into the scanning of impression materials report different and even contradictory results. One piece of research by Bosniac et al.[14] concludes that scans of conventional impressions made using laboratory scanners are inferior to those obtained using intraoral scanners when it comes to the marginal adaptation of zirconium crowns on abutments replicating natural teeth.
The authors attribute the difference to the lab scanner’s limited ability to read deep cavities, internal contours and undercut areas in impressions. Abdel-Azim et al.,[15] having tested the accuracy of impressions for producing lithium disilicate crowns, draw exactly the opposite conclusion.
Another very interesting study by Runkel et al.[16] shows that the choice of scannable or non-scannable materials greatly influences the accuracy and precision of the scan, and that scan sprays can actually cause error if applied too thickly.
Scanning dental impressions: other advantages
Another interesting possibility presented by impression scanning concerns the production of complete removable prostheses.
To have sufficient retention and stability, the base of a complete prosthesis needs to adapt extremely accurately to the supporting edentulous areas [17]. The peripheral seal must closely follow the contours of the alveolar mucosa: only in this way can the base of the prosthesis at the supporting tissues be properly isolated and the necessary suction effect produced by the saliva [5].
In this field, unlike conventional impression materials, digital impressions are not yet able to guarantee the production of a perfectly fitting removable prosthesis. This is because digital registrations of the peripheral seal area still show major discrepancies compared to even a single alginate impression [5].
Scanning errors
The absence of compression, combined with the mobility of soft tissues and the potential for stretching them, especially in vestibular areas, given the size of the probes, can cause scanning errors. In this context, scanning an analogue impression could be a convenient way to move on to the next phase and permit a digital workflow that is advantageous for both practice and patient in the production of removable prostheses.
Some research maintains that prosthetic bases produced from blocks of pre-cured resin in a CAD-CAM process are more precise and adapt better to the soft tissues of the patient than those obtained using conventional techniques because of polymerization shrinkage in the resin [18–20].
Conclusions
To conclude, scanning an impression is a valid alternative technique to intraoral scanning and may, in certain clinical cases, even afford better results.
Nevertheless, the conventional workflow validated by decades of practice, based on the production of stone models from an analogue impression, remains the “gold standard” for most rehabilitations. Stone models will therefore continue to play a fundamental role in many laboratory and clinical workflows.
Bibliography:
[1] Silva NRFA, Witek L, Coelho PG, Thompson VP, Rekow ED, Smay J. Additive CAD/CAM process for dental prostheses. J Prosthodont Off J Am Coll Prosthodont 2011;20:93–6. https://doi.org/10.1111/j.1532-849X.2010.00623.x.
[2] Chochlidakis KM, Papaspyridakos P, Geminiani A, Chen C-J, Feng IJ, Ercoli C. Digital versus conventional impressions for fixed prosthodontics: A systematic review and meta-analysis. J Prosthet Dent 2016;116:184-190.e12. https://doi.org/10.1016/j.prosdent.2015.12.017.
[3] Lim J-H, Park J-M, Kim M, Heo S-J, Myung J-Y. Comparison of digital intraoral scanner reproducibility and image trueness considering repetitive experience. J Prosthet Dent 2018;119:225–32. https://doi.org/10.1016/j.prosdent.2017.05.002.
[4] Ting-Shu S, Jian S. Intraoral Digital Impression Technique: A Review. J Prosthodont Off J Am Coll Prosthodont 2015;24:313–21. https://doi.org/10.1111/jopr.12218.
[5] D’Arienzo LF, D’Arienzo A, Borracchini A. Comparison of the suitability of intra-oral scanning with conventional impression of edentulous maxilla in vivo. A preliminary study. J Osseointegration 2018;10:115–20. https://doi.org/10.23805/jo.2018.10.04.02.
[6] Celeghin G, Franceschetti G, Mobilio N, Fasiol A, Catapano S, Corsalini M, et al. Complete-Arch Accuracy of Four Intraoral Scanners: An In Vitro Study. Healthcare 2021;9:246. https://doi.org/10.3390/healthcare9030246.
[7] Di Fiore A, Meneghello R, Graiff L, Savio G, Vigolo P, Monaco C, et al. Full arch digital scanning systems performances for implant-supported fixed dental prostheses: a comparative study of 8 intraoral scanners. J Prosthodont Res 2019;63:396–403. https://doi.org/10.1016/j.jpor.2019.04.002.
[8] Son K, Lee K-B. Prediction of learning curves of 2 dental CAD software programs, part 2: Differences in learning effects by type of dental personnel. J Prosthet Dent 2020;123:747–52. https://doi.org/10.1016/j.prosdent.2019.05.026.
[9] Ender A, Attin T, Mehl A. In vivo precision of conventional and digital methods of obtaining complete-arch dental impressions. J Prosthet Dent 2016;115:313–20. https://doi.org/10.1016/j.prosdent.2015.09.011.
[10] Quaas S, Rudolph H, Luthardt RG. Direct mechanical data acquisition of dental impressions for the manufacturing of CAD/CAM restorations. J Dent 2007;35:903–8. https://doi.org/10.1016/j.jdent.2007.08.008.
[11] Catapano S, Ferrari M, Mobilio N, Montanari M, Corsalini M, Grande F. Comparative Analysis of the Stability of Prosthetic Screws under Cyclic Loading in Implant Prosthodontics: An In Vitro Study. Appl Sci 2021;11:622. https://doi.org/10.3390/app11020622.
[12] Matta RE, Adler W, Wichmann M, Heckmann SM. Accuracy of impression scanning compared with stone casts of implant impressions. J Prosthet Dent 2017;117:507–12. https://doi.org/10.1016/j.prosdent.2016.07.026.
[13] García-Martínez I, CáceresMonllor D, Solaberrieta E, Ferreiroa A, Pradíes G. Accuracy of digitization obtained from scannable and nonscannable elastomeric impression materials. J Prosthet Dent 2021;125:300–6. https://doi.org/10.1016/j.prosdent.2020.01.002.
[14] Bosniac P, Rehmann P, Wöstmann B. Comparison of an indirect impression scanning system and two direct intraoral scanning systems in vivo. Clin Oral Investig 2019;23:2421–7. https://doi.org/10.1007/s00784-018-2679-4.
[15] Abdel-Azim T, Rogers K, Elathamna E, Zandinejad A, Metz M, Morton D. Comparison of the marginal fit of lithium disilicate crowns fabricated with CAD/CAM technology by using conventional impressions and two intraoral digital scanners. J Prosthet Dent 2015;114:554–9. https://doi.org/10.1016/j.prosdent.2015.04.001.
[16] Runkel C, Güth J-F, Erdelt K, Keul C. Digital impressions in dentistry—accuracy of impression digitalisation by desktop scanners. Clin Oral Investig 2020;24:1249–57. https://doi.org/10.1007/s00784-019-02995-w.
[17] Al-Ansari A, Tantawi ME. Patient-reported outcomes and efficiency of complete dentures made with simplified methods: A meta-analysis. Dent Med Probl 2019;56:411–8. https://doi.org/10.17219/dmp/109945.
[18] Grande F, Tesini F, Pozzan MC, Zamperoli EM, Carossa M, Catapano S. Comparison of the Accuracy between Denture Bases Produced by Subtractive and Additive Manufacturing Methods: A Pilot Study. Prosthesis 2022;4:151–9. https://doi.org/10.3390/prosthesis4020015.
[19] Hwang H-J, Lee SJ, Park E-J, Yoon H-I. Assessment of the trueness and tissue surface adaptation of CAD-CAM maxillary denture bases manufactured using digital light processing. J Prosthet Dent 2019;121:110–7. https://doi.org/10.1016/j.prosdent.2018.02.018.
[20] Wang C, Shi Y-F, Xie P-J, Wu J-H. Accuracy of digital complete dentures: A systematic review of in vitro studies. J Prosthet Dent 2021;125:249–56. https://doi.org/10.1016/j.prosdent.2020.01.004.
Do you want more information on Zhermack Dental products and solutions?
Contact us

 Zhermack SpA has been one of the most important producers and international distributors of alginates, gypsums and silicone compounds for the dental sector for over 40 years. It has also developed solutions for the industrial and wellbeing sectors.
Zhermack SpA - Via Bovazecchino, 100 - 45021 Badia Polesine (RO), Italy.
Zhermack SpA has been one of the most important producers and international distributors of alginates, gypsums and silicone compounds for the dental sector for over 40 years. It has also developed solutions for the industrial and wellbeing sectors.
Zhermack SpA - Via Bovazecchino, 100 - 45021 Badia Polesine (RO), Italy.


