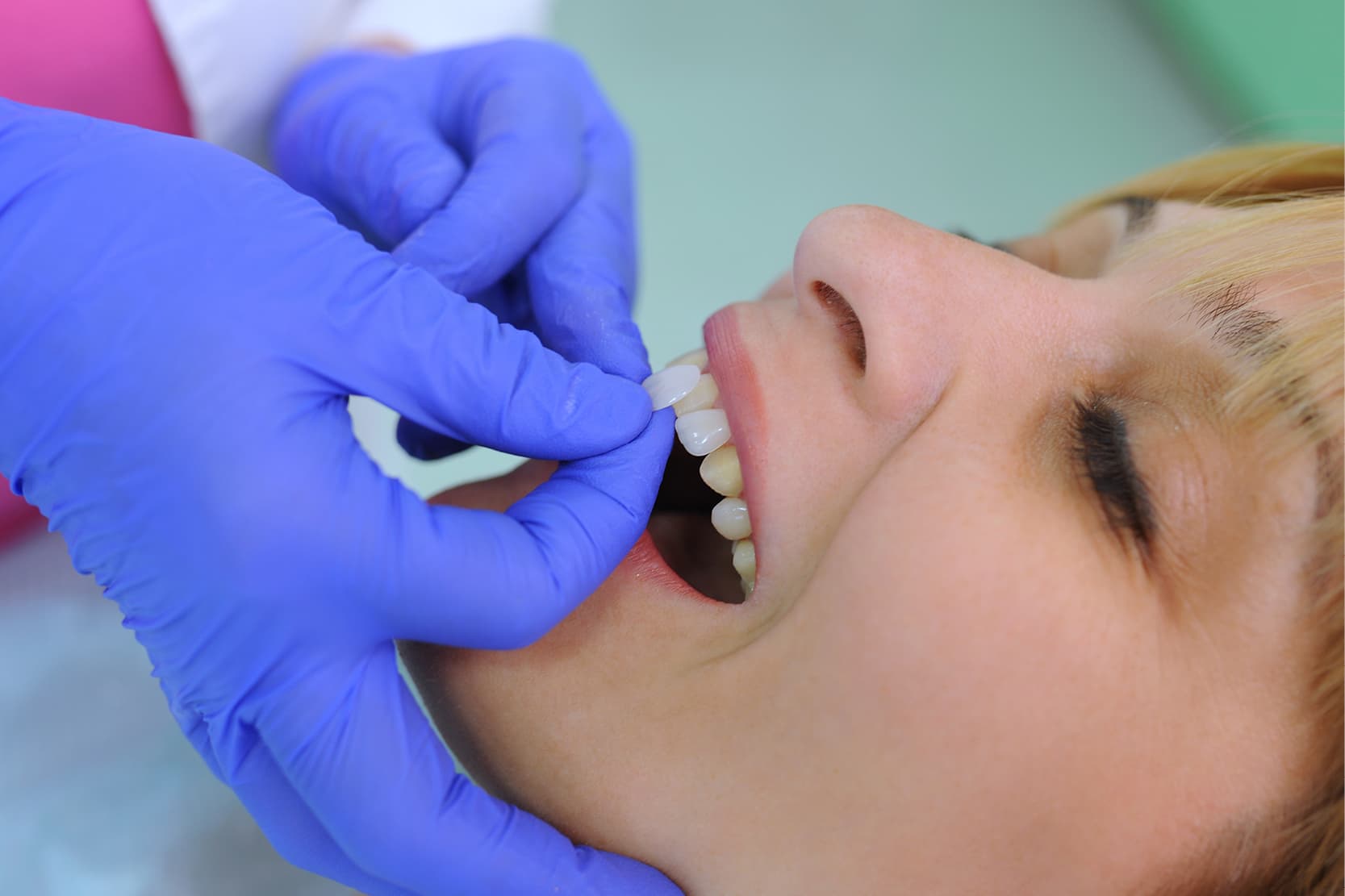
The rehabilitation of the anterior sector is one of the most demanding and risky procedures for dentists as, in most cases, these treatments are carried out on young patients with high aesthetic demands [1].
Dental veneers are very thin ceramic plates (with a thickness of 0.5-0.7 mm) that are applied to the vestibular surface of the front teeth and are therefore able to provide a good aesthetic result [2].
Ceramic and composite dental veneers
They are usually made with feldspathic ceramic or lithium disilicate, because of the excellent aesthetic performance of these materials due to their vitreous component[3]. Lithium disilicate has greater fracture strength than feldspathic ceramics [4,5]; the disilicate crystals are closely interconnected and surrounded by the glass matrix, affording greater fracture energy absorption and increasing the resistance and tenacity of the material[6].
Some dentists also use composites or cubic zirconia for these restorations. Being a polycrystalline ceramic, zirconia is a material with a greater fracture strength than glass-matrix ceramics[7]. It can be worked using CAD-CAM technology only and, in the monolithic form it is opaque [8], making it possible to conceal significant colour differences and abutment reconstructions using metal pins.
Composite materials are also more opaque than glass-matrix ceramics and have the added advantage of being easy to adjust using additive techniques [9]. However, in addition to the poorer cosmetic result compared to glass-matrix ceramics [10], these materials also have other drawbacks. Given their porous structure, [11] composites tend to absorb pigments over time, which alter the colour of the restoration. Cubic zirconia, on the other hand, presents bonding problems with resin-based luting cements[12].
Preparing ceramic dental veneers
According to Magne and Belser[13], ceramic veneers are a tried-and-tested, effective and predictable treatment option when whitening is insufficient for obtaining the desired aesthetic result and when significant morphological changes (conoid teeth) and extensive restorations are required in adult patients.
The clinical/laboratory procedures required for the preparation of ceramic dental veneers can be broken down into 8 steps[14]:
- Intra- and extraoral aesthetic analysis of the patient, with photographs of the case and initial impressions;
- Digital preview using DSS (Digital Smile System), DSD (Digital Smile Design) or a diagnostic wax-up and patient’s approval;
- Clinical preview by fabricating mock-ups or an aesthetic temporary restoration, based on a wax-up on a gypsum model or a virtual wax-up;
- Assessment and treatment of root canal, mucogingival and/or orthodontic problems, where necessary;
- Preparation of the teeth based on the mock-up;
- Secondary impression;
- Fabrication of the veneers by the dental technician;
- Fitting and cementation of the veneers under dental rubber dam isolation.
Veneer preparation and cementation techniques
In order to provide an aesthetic and functional rehabilitation, the prosthetic preparation of the teeth for the veneers must comply with the concepts of minimal invasiveness introduced with bonding [15] in modern Prosthetic and Conservative Dentistry. Furthermore, it is essential that no errors that might prejudice the end result are committed in the final veneer cementationstep (add internal link to the “Dental veneer cementation”).
A number of different methods have therefore been put forward for the preparation of the incisal edge (bevelled, butt joint and palatal chamfer)[16], vestibular surface (guide groove and/or silicone index technique) and interproximal portions of the teeth[17]. In addition, in some cases, it is not necessary to prepare the teeth (“no prep technique”) [18].
Subsequently, during the phases of cementing, under a dental rubber dam[19], it is important not to lose sight of the aesthetic landmarks, in order to ensure a correct spatial positioning of the veneers on the teeth[20].
And, last but by no means least, the correct use of impression materials within a precise, standardised workflow[21].
Conclusions
To conclude, it can therefore be said that dental veneers represent an aesthetic and, to a certain extent, also functional treatment.
The clinical procedures for their fabrication involve a series of mandatory steps and the use of a plethora of materials and specific techniques in order to obtain an aesthetic result that is satisfactory for the dentist and, above all, for the patient.
Bibliography:
[1] Edelhoff D, Prandtner O, Saeidi Pour R, Liebermann A, Stimmelmayr M, Güth J-F. Anterior restorations: The performance of ceramic veneers. Quintessence Int Berl Ger 1985 2018;49:89–101. https://doi.org/10.3290/j.qi.a39509.
[2] Fradeani M, Redemagni M, Corrado M. Porcelain laminate veneers: 6- to 12-year clinical evaluation–a retrospective study. Int J Periodontics Restorative Dent 2005;25:9–17.
[3] AlJazairy YH. Survival Rates for Porcelain Laminate Veneers: A Systematic Review. Eur J Dent 2021;15:360–8. https://doi.org/10.1055/s-0040-1715914.
[4] Grande F, Mochi Zamperoli E, Pozzan MC, Tesini F, Catapano S. Qualitative Evaluation of the Effects of Professional Oral Hygiene Instruments on Prosthetic Ceramic Surfaces. Materials 2021;15:21. https://doi.org/10.3390/ma15010021.
[5] Mobilio N, Fasiol A, Catapano S. Survival Rates of Lithium Disilicate Single Restorations: A Retrospective Study. Int J Prosthodont 2018;31:283–6. https://doi.org/10.11607/ijp.5601.
[6] Baldi A, Comba A, Michelotto Tempesta R, Carossa M, Pereira GKR, Valandro LF, et al. External Marginal Gap Variation and Residual Fracture Resistance of Composite and Lithium-Silicate CAD/CAM Overlays after Cyclic Fatigue over Endodontically-Treated Molars. Polymers 2021;13:3002. https://doi.org/10.3390/polym13173002.
[7] Nakamura T, Nakano Y, Usami H, Okamura S, Wakabayashi K, Yatani H. In vitro investigation of fracture load and aging resistance of high-speed sintered monolithic tooth-borne zirconia crowns. J Prosthodont Res 2020;64:182–7. https://doi.org/10.1016/j.jpor.2019.07.003.
[8] Tuncel İ, Turp I, Üşümez A. Evaluation of translucency of monolithic zirconia and framework zirconia materials. J Adv Prosthodont 2016;8:181–6. https://doi.org/10.4047/jap.2016.8.3.181.
[9] Demarco FF, Collares K, Coelho-de-Souza FH, Correa MB, Cenci MS, Moraes RR, et al. Anterior composite restorations: A systematic review on long-term survival and reasons for failure. Dent Mater Off Publ Acad Dent Mater 2015;31:1214–24. https://doi.org/10.1016/j.dental.2015.07.005.
[10] Daneshpooy M, Pournaghi Azar F, Alizade Oskoee P, Bahari M, Asdagh S, Khosravani SR. Color agreement between try-in paste and resin cement: Effect of thickness and regions of ultra-translucent multilayered zirconia veneers. J Dent Res Dent Clin Dent Prospects 2019;13:61–7. https://doi.org/10.15171/joddd.2019.010.
[11] Berge M, Hegdahl T. Porosity of resin veneer materials. Acta Odontol Scand 1987;45:321–8. https://doi.org/10.3109/00016358709096354.
[12] Quigley NP, Loo DSS, Choy C, Ha WN. Clinical efficacy of methods for bonding to zirconia: A systematic review. J Prosthet Dent 2021;125:231–40. https://doi.org/10.1016/j.prosdent.2019.12.017.
[13] Magne P, Belser U. Bonded Porcelain Restorations in the Anterior Dentition: A Biomimetic Approach. Chicago: Quintessence, 2002. n.d.
[14] Ortensi L, Vitali T, Bonfiglioli R, Grande F. New Tricks in the Preparation Design for Prosthetic Ceramic Laminate Veeners. Prosthesis 2019;1:29–40. https://doi.org/10.3390/prosthesis1010005.
[15] Pereira JR, Pamato S, Vargas M, Junior NF. State of the Art of Dental Adhesive Systems. Curr Drug Deliv 2018;15:610–9. https://doi.org/10.2174/1567201814666171120120935.
[16] da Costa DC, Coutinho M, de Sousa AS, Ennes JP. A meta-analysis of the most indicated preparation design for porcelain laminate veneers. J Adhes Dent 2013;15:215–20. https://doi.org/10.3290/j.jad.a29587.
[17] Abuzenada B, Alanazi A, Saydali W, Elmarakby A, Koshak H, Alharthi A. Current classifications and preparation techniques of dental ceramic laminate veneers (Review article). Int J Adv Res 2017;5(12):1973-1979 n.d.
[18] Wells DJ. “No-prep” veneers. Inside Dent. 2010; 6(8):56-60 n.d.
[19] Miao C, Yang X, Wong MC, Zou J, Zhou X, Li C, et al. Rubber dam isolation for restorative treatment in dental patients. Cochrane Database Syst Rev 2021;5:CD009858. https://doi.org/10.1002/14651858.CD009858.pub3.
[20] Mizrahi B. Porcelain veneers: techniques and precautions. Internal Dent, 2007;9(6):1-4. n.d.
[21] Ahlholm P, Sipilä K, Vallittu P, Jakonen M, Kotiranta U. Digital Versus Conventional Impressions in Fixed Prosthodontics: A Review. J Prosthodont Off J Am Coll Prosthodont 2018;27:35–41. https://doi.org/10.1111/jopr.12527.
Do you want more information on Zhermack Dental products and solutions?
Contact us


 Zhermack SpA has been one of the most important producers and international distributors of alginates, gypsums and silicone compounds for the dental sector for over 40 years. It has also developed solutions for the industrial and wellbeing sectors.
Zhermack SpA - Via Bovazecchino, 100 - 45021 Badia Polesine (RO), Italy.
Zhermack SpA has been one of the most important producers and international distributors of alginates, gypsums and silicone compounds for the dental sector for over 40 years. It has also developed solutions for the industrial and wellbeing sectors.
Zhermack SpA - Via Bovazecchino, 100 - 45021 Badia Polesine (RO), Italy.


