
Working in the dental sector implies the use of professional tools that can expose healthcare professionals and patients to a constant risk of direct and cross-infection. In addition, the oral cavity houses a high quantity of different bacterial species, which favours and increases the risk of infection.
Dental practice environments can be an important route for the transmission of infectious diseases, for both the dental team and the patient[1]. Each time new infectious diseases are discovered, the protocols for controlling infection in the dental healthcare sector are amended accordingly[2], [3]
Cross-infection: the main routes of transmission
Cross-infection can be defined as the transmission of infectious agents between patients and staff inside a clinical environment.
Transmission may be due to person-to-person contact or contaminated objects. The transmission of the infection from one person to another requires a source of infection. Infectious agents are transmitted through blood saliva droplets and instruments contaminated by blood, saliva and tissue fragments.
The main routes of transmission can be inhalation or inoculation[4], but also contact. More specifically, transmission can take place:
- Through transmission by direct contact, i.e. as a result of direct contact between an individual able to infect (sick or colonised person or healthy carrier) and a healthy individual;
- Through transmission by indirect contact, i.e. as a result of contact with contaminated surfaces, equipment or inanimate objects;
- Through transmission by the diffusion of nucleic droplets, as well as through the respiratory tract and oral cavity after sneezing or coughing etc., when particles of varying sizes and that can contain infectious microorganisms are released.
In dentistry, the sources of infection can be patients with infectious diseases or healthy carriers of pathogenic agents.
Carriers of pathogenic agents that pose a threat of disease transmission can be classified as asymptomatic carriers.Asymptomatic carriers do not have a past history of infection, since they may have unknowingly had a subclinical infection and therefore they can be difficult to identify and may carry pathogenic microorganisms in their saliva and blood.
Hepatitis B is a classic example of an illness that can present with or without symptoms[5].
Transmission of infections inside dental practices
Inside dental practices, infections can be transmitted by direct contact with secretions or blood, through droplets containing infectious agents or by contaminated sharp instruments that have not be properly sterilised.
The main route of cross-contamination in oral surgery associated with sharp objects or direct contact between infectious agents and broken skin or grazes[6] [7].
Viral diseases such as hepatitis B, acquired immune deficiency syndrome (AIDS), herpes simplex and cytomegalovirus pose significant risks, not only for dentists but also for their families, friends and other patients[8] [9].
Protective barriers for controlling infection
Use of gloves by dental staff is recommended as an essential element for the control of cross-infection during dental surgery[10] [11].
Oral surgery assistants, who are involved in the treatment of patients, cleaning and surgical disinfection, should wear gloves, as their hands are considered one of the main sources of infection[12] and potentially infected blood can remain under fingernails for up to five days[13].
Protective barriers act by protecting the practitioner from the patients and vice versa, or both from the contaminated surrounding environment. These barriers include gloves, face masks, eye protection, tray covers, and covers for worktops and the surrounding objects at risk of contamination[14] [15].
It is the practitioner’s duty to ensure that all members of the dental team are adequately trained and equipped to perform effective control of cross-infection, not only to optimise the protection of all dental practice staff, but also to prevent the spread of infection from one patient to another[16] [17] [18] [19].
Zhermack’s Zeta Hygiene line provides a range of disinfectants and detergents with a broad spectrum of action in concentrated liquid form (Zeta 1 Ultra), specifically intended for the disinfection of ordinary and surgical dental instruments and burs, or in powder form (Zeta 2 Sporex), specifically intended for the treatment of instruments prior to sterilisation, even for medical devices that cannot be autoclaved.
Bibliography
[1] Volgenant, C., & de Soet, J. (2018). Cross-transmission in the dental office: Does this make you ill? Current Oral Health Reports, 5(4), 221–228. https://doi.org/10.1007/s40496-018-0201-3
[2] Monaghan, N. P. (2016). Emerging infections – implications for dental care. British Dental Journal, 221(1), 13–15. https://doi.org/10.1038/sj.bdj.2016.486
[3] Smales, F. C., & Samaranyake, L. P. (2003). Maintaining dental education and specialist dental care during an outbreak of a new coronavirus infection. Part 2: Control of the disease, then elimination. British Dental Journal, 195(12), 679–681. https://doi.org/10.1038/sj.bdj.4810819
[4] Verrusio AC et al. The dentist and infectious diseases: a national survey of attitudes and behavior. Journal of the American Dental Association, 1989, 118:553-62.
[5] note no. 4
[6] note no. 4
[7] Girdler NM, Matthews RW, Scully C. Use and acceptability of rubber gloves for outpatient dental treatment. Journal of dentistry, 1987, 15:209-212.
[8] Walkinson AC. Primary herpes simplex in a dentist. British dental journal, 1982, 153:190-1.
[9] Sins W. The problem of cross infection in dental hepatitis with particular reference to serum hepatitis. Journal of dentistry, 1980, 8:20-6.
[10] Rustage KJ, Rothwell PS, Brook IM. Evaluation of a dedicated dental procedure glove for clinical dentistry. British dental journal, 1987, 103:193-5.
[11] Crawford TJ. State of the art practical infection control in dentistry. Journal of the American Dental Association, 1985, 110:629-33.
[12] Burke FJT, Wilson NHF and Bogge HFJ. Glove wearing by dental surgery assistants. Dental update, 1993, 20:385-7
[13] Allen AL and Organ RJ. Occult blood accumulation under the finger nails. A mechanism for the spread of blood borne infection. Journal of the American Dental Association, 1982, 105:455-9.
[14] come nota 15
[15] Croser D. Infection control—the dental perspective. Dental health, 1991, 30(6):92-6.
[16] come nota 11
[17] Cowan DDJ. Infection control in general dental practice. British dental journal, 1987, 162:292-7.
[18] Martin MV. Infection control in general dental practice. British dental journal, 162:37-8.
[19] Samaranayake LP. Infection control in general dental practice. British dental journal, 1987, 162:413-4.
Would you like information about Zhermack products and dental solutions?
Contact us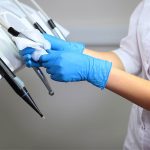



 Zhermack SpA has been one of the most important producers and international distributors of alginates, gypsums and silicone compounds for the dental sector for over 40 years. It has also developed solutions for the industrial and wellbeing sectors.
Zhermack SpA - Via Bovazecchino, 100 - 45021 Badia Polesine (RO), Italy.
Zhermack SpA has been one of the most important producers and international distributors of alginates, gypsums and silicone compounds for the dental sector for over 40 years. It has also developed solutions for the industrial and wellbeing sectors.
Zhermack SpA - Via Bovazecchino, 100 - 45021 Badia Polesine (RO), Italy.


