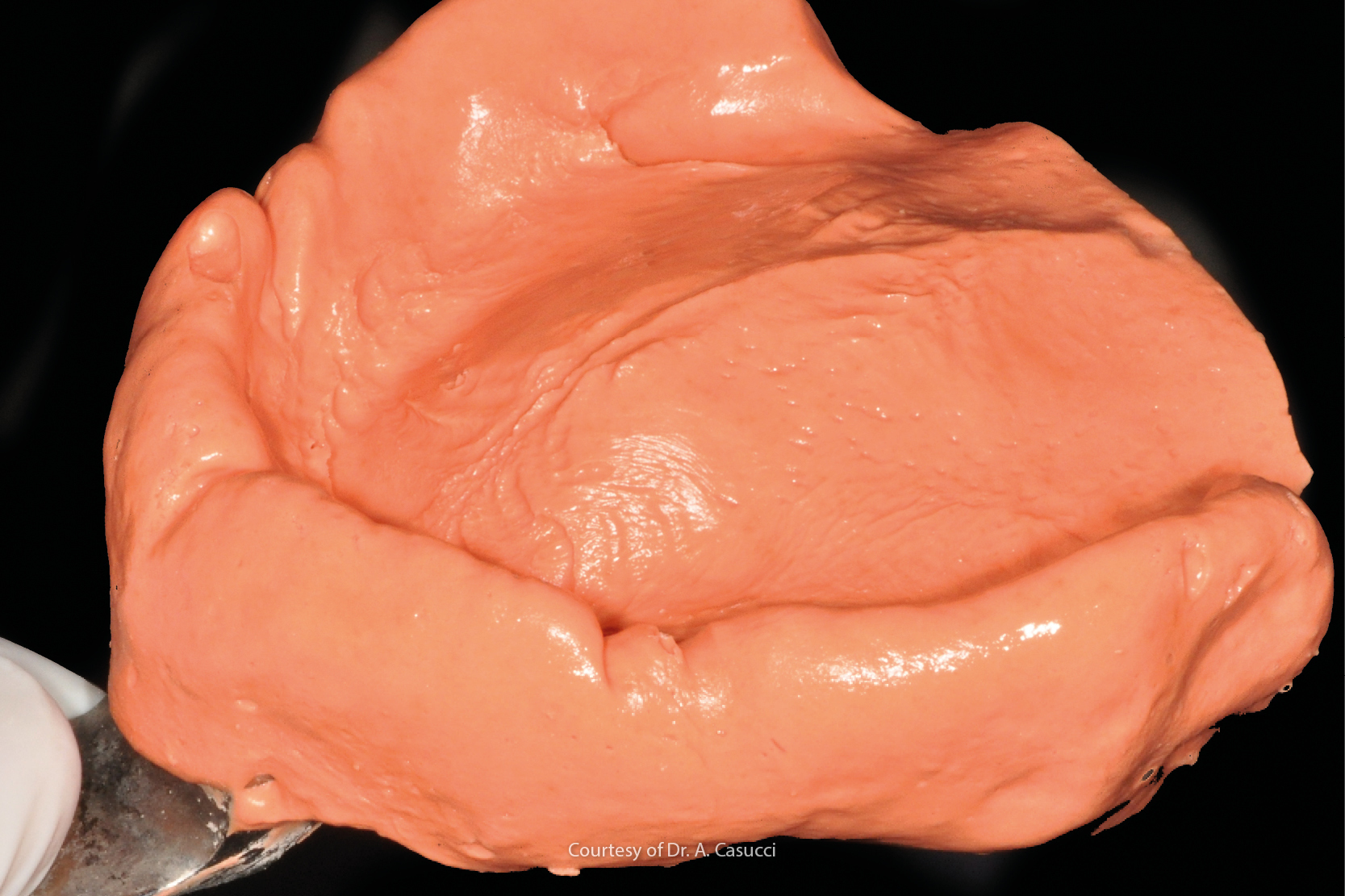
Alginates are the most frequently used of all impression materials in dental practices [1]. They are essential in daily clinical procedures in all branches of dentistry that require collaboration between dentist and dental technician.
Alginate impressions are extremely quick and easy to take, and mixing is simple and rapid too. No special equipment is needed and the materials are inexpensive and well tolerated by most patients [1].
Physico-chemical characteristics of the alginates
Furthermore, since alginates are irreversible hydrocolloids formed from the sodium and potassium salts of alginic acid, they also have certain useful chemical and physical properties:
- first of all, they are hydrophilic and therefore perform well in contact with water and oral mucosa which are often wet with saliva;
- secondly, they are perfectly compatible with the gypsum used for preparing the models on which prostheses are made;
- finally, they generally have short setting times, though types offering extended times are also available (e.g. Zhermack’s Neocolloid has a long setting time to permit proper functionalisation of the frenums, essential to identifying the limits of future removable prostheses /custom impression trays) [2–4].
Uses of alginates
In the vast majority of cases, alginates are used for preliminary / primary impressions and for temporary prostheses or models. Some practitioners, however, also find them useful as the final impression material for removable prostheses [5].
In normal clinical work, many dentists have adopted simplified procedures [6,7]. It seems that such simplification is indeed useful especially for practitioners with less experience: an in vivo study has shown that teaching an abbreviated technique for producing a complete prosthesis (with just one alginate impression instead of two) in a university surgery resulted in a lower number of appointments being needed to deliver the finished prosthesis without any increase in the number of post-fitting adjustments or modifications [6].
The impression phase in the production of a complete prosthesis allows the base to be customised in order to ensure an optimal area of support and a shape that forms a perfect peripheral seal. This is the only way to ensure the stability and retention needed to obtain a fully functional prosthesis [8].
When producing a removable prosthesis, therefore, it is essential to obtain an extremely accurate impression of the patient’s soft tissues as well as the correct extension of the fornix and the relevant frenums and post dam. This is often difficult with a single impression and, though there is a wide range of variation in preferences for a particular material or technique, most dentistry schools teach that at least two impressions are needed to obtain an acceptable result [8].
To prove the point, Hyde et al. in 2014 showed in an RCT involving 85 totally edentulous patients, complete prostheses made from two impressions (first alginate and then silicone) were preferred by more patients (67.9%) to those produced from a single alginate impression [9]. Nevertheless, the patients found both types of prosthesis, including those produced from a single alginate impression, quite satisfactory. This finding is certainly influenced by various factors, including the degree of patient acceptance and neuromuscular control, etc. [10,11] but it certainly confirms the effectiveness of alginates as impression materials for complete prostheses.
A review of the literature that attempts to identify the best impression taking material and technique for use with complete prostheses concluded that prosthesis production based on a single alginate impression taken with a standard impression tray satisfies the needs of most edentulous patients [8]. This is quite understandable if we consider the fact that the success of the prosthesis depends more on patient acceptance than on the absolute quality of the prosthesis itself [11–14]. Furthermore, the majority of edentulous patients do not necessarily have severe osseous resorption. This guarantees reasonable undercut areas that give the removable prosthesis good retention.
The reasons why alginates are frequently used to produce removable prostheses and are always preferred for the primary impression are explained by the materials’ hydrophilia and mucostaticity. These properties produce an overextended impression that ensures that the frenums, post dam and depth of the vestibule are clearly visible in the stone model. Such anatomic details enable the dental technician to mark the limits of the future complete prosthesis or, in the case of a double step impression, to produce a more suitable custom impression tray.
Conclusions
In any case, it is difficult to contest the “Appropriatech” concept put forward by Owen [15], according to which dentists should use the simplest and least expensive methods and materials to deliver qualitatively acceptable prostheses for the largest number of edentulous patients. However, it is also true that each case is unique and that there is a great deal of variation between patients. Ultimately, of course, the practitioner must choose both material and technique to suit the patient if he is to ensure the production of a complete removable prosthesis of good quality and acceptability.
Zhermack supplies a wide range of alginates for use in the production of partial and complete removable prostheses for partly and totally edentulous patients. In particular, Neocolloid is an alginate with a long setting time, and is formulated to obtain a good impression of an edentulous patient’s mucosa. Thanks to Neocolloid’s physical and chemical properties, accurate reproduction of the maxillary mucosa is guaranteed.
References:
[1] Cervino G, Fiorillo L, Herford AS, Laino L, Troiano G, Amoroso G, et al. Alginate Materials and Dental Impression Technique: A Current State of the Art and Application to Dental Practice. Mar Drugs 2018;17. https://doi.org/10.3390/md17010018.
[2] Murata H, Kawamura M, Hamada T, Chimori H, Nikawa H. Physical properties and compatibility with dental stones of current alginate impression materials. J Oral Rehabil 2004;31:1115–22. https://doi.org/10.1111/j.1365-2842.2004.01343.x.
[3] Dilip A, Gupta R, Geiger Z. Dental Alginate Impressions. StatPearls, Treasure Island (FL): StatPearls Publishing; 2021.
[4] Craig RG. Review of dental impression materials. Adv Dent Res 1988;2:51–64. https://doi.org/10.1177/08959374880020012001.
[5] Punj A, Bompolaki D, Garaicoa J. Dental Impression Materials and Techniques. Dent Clin North Am 2017;61:779–96. https://doi.org/10.1016/j.cden.2017.06.004.
[6] Duncan JP, Taylor TD. Teaching an abbreviated impression technique for complete dentures in an undergraduate dental curriculum. J Prosthet Dent 2001;85:121–5. https://doi.org/10.1067/mpr.2001.113699.
[7] Gauthier G, Williams JE, Zwemer JD. The practice of complete denture prosthodontics by selected dental graduates. J Prosthet Dent 1992;68:308–13. https://doi.org/10.1016/0022-3913(92)90335-8.
[8] Carlsson GE, Örtorp A, Omar R. What is the evidence base for the efficacies of different complete denture impression procedures? A critical review. Journal of Dentistry 2013;41:17–23. https://doi.org/10.1016/j.jdent.2012.11.015.
[9] Hyde TP, Craddock HL, Gray JC, Pavitt SH, Hulme C, Godfrey M, et al. A Randomised Controlled Trial of complete denture impression materials. Journal of Dentistry 2014;42:895–901. https://doi.org/10.1016/j.jdent.2014.02.005.
[10] Ettinger RL. Treatment planning concepts for the ageing patient. Aust Dent J 2015;60 Suppl 1:71–85. https://doi.org/10.1111/adj.12286.
[11] Friedman N, Landesman HM, Wexler M. The influences of fear, anxiety, and depression on the patient’s adaptive responses to complete dentures. Part I. J Prosthet Dent 1987;58:687–9. https://doi.org/10.1016/0022-3913(87)90419-7.
[12] Närhi TO, Ettinger RL, Lam EW. Radiographic findings, ridge resorption, and subjective complaints of complete denture patients. Int J Prosthodont 1997;10:183–9.
[13] Diehl RL, Foerster U, Sposetti VJ, Dolan TA. Factors associated with successful denture therapy. J Prosthodont 1996;5:84–90. https://doi.org/10.1111/j.1532-849x.1996.tb00279.x.
[14] Carlsson GE, Otterland A, Wennström A, Odont D. Patient factors in appreciation of complete dentures. J Prosthet Dent 1967;17:322–8. https://doi.org/10.1016/0022-3913(67)90002-9.
[15] Owen PC. Appropriatech: prosthodontics for the many, not just for the few. Int J Prosthodont 2004;17:261–2.
Do you want more information on Zhermack Dental products and solutions?
Contact Us

 Zhermack SpA has been one of the most important producers and international distributors of alginates, gypsums and silicone compounds for the dental sector for over 40 years. It has also developed solutions for the industrial and wellbeing sectors.
Zhermack SpA - Via Bovazecchino, 100 - 45021 Badia Polesine (RO), Italy.
Zhermack SpA has been one of the most important producers and international distributors of alginates, gypsums and silicone compounds for the dental sector for over 40 years. It has also developed solutions for the industrial and wellbeing sectors.
Zhermack SpA - Via Bovazecchino, 100 - 45021 Badia Polesine (RO), Italy.


