14
Nov
Fixed prostheses supported by multiple implants: technical procedures for fabrication
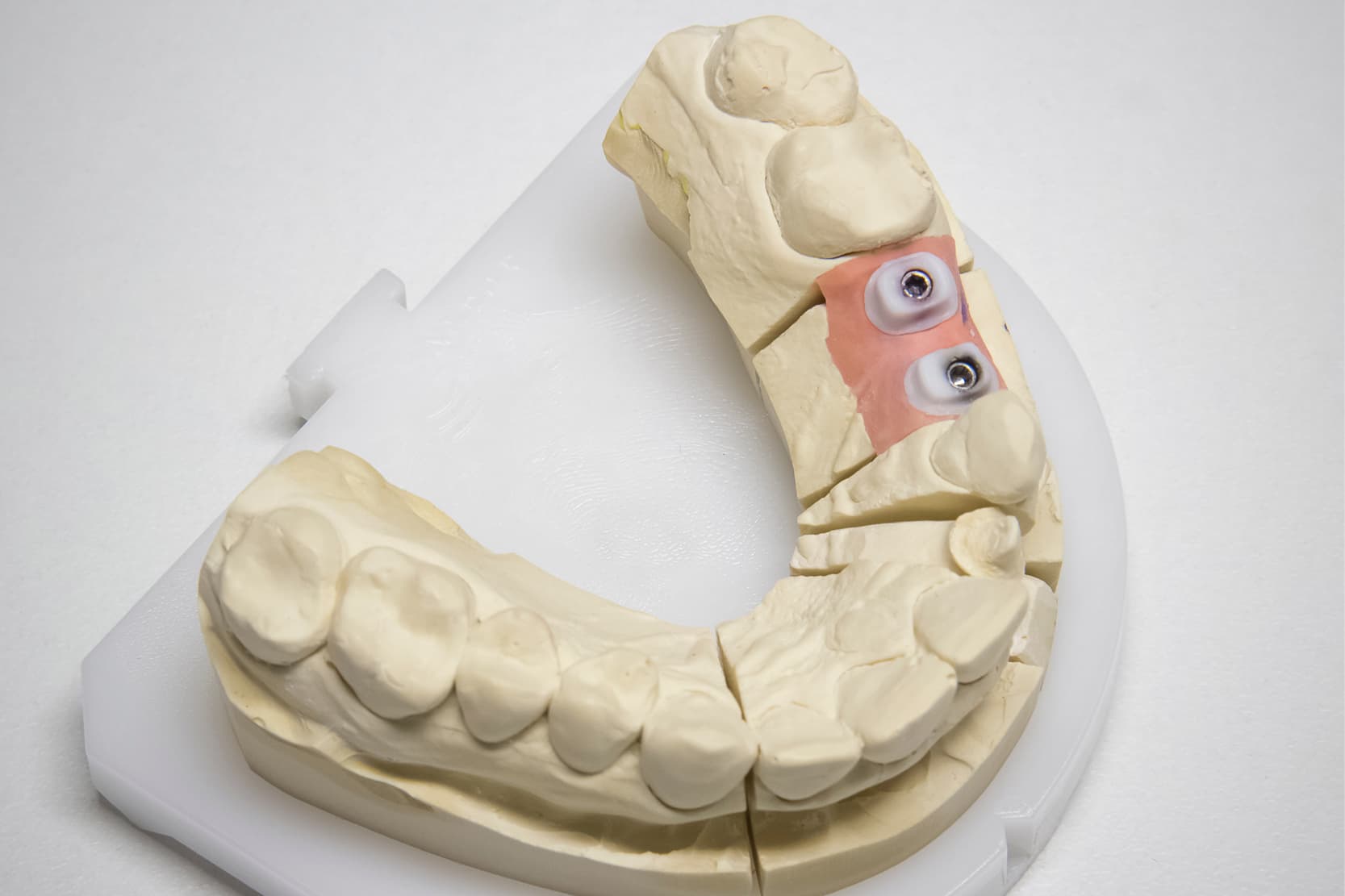
The literature provides ample evidence that the technical procedure for the fabrication of fixed prostheses supported by multiple implants are fundamental phases for determining the success of restoration [1–3].
This article therefore analyses the technical procedures inherent to the fabrication of fixed prostheses supported by multiple implants, in order to clarify an area that is often underestimated by dentists.
Foreword
It should be immediately pointed out that the technical phases for the fabrication of this type of prosthesis can vary depending on the clinical case and the type of restoration [4–7].
Furthermore, with digital technologies, the entire process becomes more complex, because the workflows multiply [8,9].
In an attempt to put things into order, however, it is possible to identify a common guideline for analogical, analogical/digital and full-digital processes.
Firstly, it can be said that laboratory workflows always start with an impression on the implants/MUA, which can be taken using conventional materials or an intraoral scanner.
This is essentially the starting point for all the phases listed in the next section.
The six phases of fabrication
1. Attainment of the master model with the implant analogues and of the antagonist model and articulation.
The models can be made of gypsum, 3D printed resin or fully-digital and they can be articulated using a mechanical or digital articulator.
2. The fabrication of a verification jig in an inflexible material, usually gypsum, which connects the implant/MUA analogues to the gypsum of 3D printed master model.
The dentist will test this jig in the patient’s mouth then send it back to the dental technician to test the congruence between the laboratory model and the clinical situation. It should be pointed out that, with a full-digital workflow, this phase can only be carried out using millable materials (aluminium or cobalt-chromium bars), which are not, however, always absolutely faithful, because they can flex after they have been screwed into the patient’s mouth [9,10].
3. Wax-up (analogue or digital).
During this step, the dentist creates physically (using wax) or digitally using the CAD programme, the design of the framework that connects the implant/MUA analogues to one another.
4. Fabrication of the framework using analogue or digital techniques.
By far the most common analogue technique is lost-wax casting, which is still extensively used to fabricate metal frameworks using different alloys (such as cobalt-chromium).
Amongst the digital techniques, on the other hand, we find additive and subtractive technologies.
Amongst the former, selective laser melting is undoubtedly the most commonly used 3D printing technique for metals. It consists in fabricating a solid structure using a high-power laser, which melts a bed of metal powder layer by layer [11].
The subtractive techniques, on the other hand, involve obtaining the framework from a solid block of industrially pre-cast material [8].
In all cases, however, this framework is tested in the patient’s mouth to confirm the passive fit on the connections, both clinically and radiographically, using the Sheffield Test [1]. The inaccuracy of prostheses on implants is known to increase the risk of mechanical complications such as the loss of fixation screw preload, the failure of the screws or intermediate abutments, chipping and investment material failure [1,12,13].
Although to date there is still no certain evidence supporting the fact that the presence of structural tensions can also increase the risk of biological complications (mucositis, peri-implantitis), passive framework fit is a factor to be sought in multiple-implant rehabilitations [14].
Therefore, whenever a framework is found not to be passive, this step must be repeated, using the information the dentist will give to the dental technician regarding the proper position of the implants/intermediate abutments.
5. Application of the investment material to the framework, when applicable [2].
In this step, the dental technician applies resin or ceramic to the framework, depending on the type of material chosen by the dentist.
It is interesting to note that this step can also introduce discrepancies in terms of the precision of the framework on the connections. Indeed, it has been demonstrated that applying ceramic to metal frameworks can generate discrepancies in the implant-prosthesis connections that are even greater than those resulting from digital framework fabrication techniques (selective laser melting, milling) [2].
Although these errors do not appear to be clinically significant, it is nevertheless appropriate to consider this factor in the light of what was said previously regarding the passive fit of the framework. Therefore, during the bar passive fit test, the structure should be well-adapted to the implants beneath.
6. Trimming and polishing of the final restoration.
In this step, the dental technician must take great care to polish the prosthesis properly, not only with regard to the investment material, but also with regard to the framework material that, at the connections, often comes into contact with the patient’s soft tissues and constitutes a potential site for the buildup of plaque and biofilm [15,16].
Conclusions
In summary, it can be said that there are various technical steps for the fabrication of a fixed prosthesis on multiple implants and they can be extremely complex if we consider the different workflows.
Today’s dental technicians must be able to combine their expertise regarding materials and conventional fabrication techniques with current workflows and with new digital production techniques, in order to ensure the dentist and the patient a flawless restoration.
Zhermack offers several high-performance products for the fabrication of gypsum models.
Elite Dental Stones is the wide range of Zhermack gypsums, with low expansion, able to satisfy the diverse requirements of dental technicians.
With its type 3 and type 4 gypsums, Elite Dental Stonesprovides specific and separate solutions, ranging from the fabrication of antagonist models to the development of master models.
References
[1] Rutkunas V, Dirse J, Kules D, Mischitz I, Larsson C, Janda M. Misfit simulation on implant prostheses with different combinations of engaging and nonengaging titanium bases. Part 2: Screw resistance test. J Prosthet Dent 2022:S0022-3913(22)00286-4. https://doi.org/10.1016/j.prosdent.2022.04.027.
[2] Revilla-León M, Sánchez-Rubio JL, Pérez-López J, Rubenstein J, Özcan M. Discrepancy at the implant abutment-prosthesis interface of complete-arch cobalt-chromium implant frameworks fabricated by additive and subtractive technologies before and after ceramic veneering. J Prosthet Dent 2021;125:795–803. https://doi.org/10.1016/j.prosdent.2020.03.018.
[3] Thakur J, Parlani S, Shivakumar S, Jajoo K. Accuracy of marginal fit of an implant-supported framework fabricated by 3D printing versus subtractive manufacturing technique: A systematic review and meta-analysis. J Prosthet Dent 2023;129:301–9. https://doi.org/10.1016/j.prosdent.2021.05.010.
[4] Lops, D., Bruna, E., & Fabianelli, A. (2014). La protesi implantare. Dental Cadmos, 6(82), 386. n.d.
[5] Ortensi L, Ortensi M, Minghelli A, Grande F. Implant-Supported Prosthetic Therapy of an Edentulous Patient: Clinical and Technical Aspects. Prosthesis 2020;2:140–52. https://doi.org/10.3390/prosthesis2030013.
[6] Pellegrino G, Basile F, Relics D, Ferri A, Grande F, Tarsitano A, et al. Computer-Aided Rehabilitation Supported by Zygomatic Implants: A Cohort Study Comparing Atrophic with Oncologic Patients after Five Years of Follow-Up. JCM 2020;9:3254. https://doi.org/10.3390/jcm9103254.
[7] Ovchinnik V, Karatas B, Yilmaz B, McGlumphy EA. Fabrication of an implant-supported fixed complete denture using multiple digital technologies for a patient with a perioral burn: A clinical report. The Journal of Prosthetic Dentistry 2018;120:161–7. https://doi.org/10.1016/j.prosdent.2017.10.026.
[8] Masri R, Driscoll C. Odontoiatria digitale: Presupposti teorici e applicazioni cliniche. Edra; 2017.
[9] Alghazzawi TF. Advancements in CAD/CAM technology: Options for practical implementation. Journal of Prosthodontic Research 2016;60:72–84. https://doi.org/10.1016/j.jpor.2016.01.003.
[10] Anusavice KJ, Shen C, Rawls HR. Phillips’ science of dental materials. 12th edition. Elsevier Health Sciences; 2012.
[11] Revilla-León M, Sadeghpour M, Özcan M. A Review of the Applications of Additive Manufacturing Technologies Used to Fabricate Metals in Implant Dentistry. Journal of Prosthodontics 2020;29:579–93. https://doi.org/10.1111/jopr.13212.
[12] Ortorp A, Jemt T, Wennerberg A, Berggren C, Brycke M. Screw preloads and measurements of surface roughness in screw joints: an in vitro study on implant frameworks. Clin Implant Dent Relat Res 2005;7:141–9. https://doi.org/10.1111/j.1708-8208.2005.tb00058.x.
[13] Jemt T. A retro-prospective effectiveness study on 3448 implant operations at one referral clinic: A multifactorial analysis. Part II: Clinical factors associated to peri-implantitis surgery and late implant failures. Clin Implant Dent Relat Res 2017;19:972–9. https://doi.org/10.1111/cid.12538.
[14] Goodacre CJ, Bernal G, Rungcharassaeng K, Kan JYK. Clinical complications with implants and implant prostheses. J Prosthet Dent 2003;90:121–32. https://doi.org/10.1016/S0022-3913(03)00212-9.
[15] Batak B, Çakmak G, Johnston WM, Yilmaz B. Surface roughness of high-performance polymers used for fixed implant-supported prostheses. The Journal of Prosthetic Dentistry 2021;126:254.e1-254.e6. https://doi.org/10.1016/j.prosdent.2020.11.029.
[16] Bollen CML, Papaioanno W, Van Eldere J, Schepers E, Quirynen M, Van Steenberghe D. The influence of abutment surface roughness on plaque accumulation and peri-implant mucositis. Clinical Oral Implants Research 1996;7:201–11. https://doi.org/10.1034/j.1600-0501.1996.070302.x.
Do you want more information on Zhermack Dental products and solutions?
Contact us

 Zhermack SpA has been one of the most important producers and international distributors of alginates, gypsums and silicone compounds for the dental sector for over 40 years. It has also developed solutions for the industrial and wellbeing sectors.
Zhermack SpA - Via Bovazecchino, 100 - 45021 Badia Polesine (RO), Italy.
Zhermack SpA has been one of the most important producers and international distributors of alginates, gypsums and silicone compounds for the dental sector for over 40 years. It has also developed solutions for the industrial and wellbeing sectors.
Zhermack SpA - Via Bovazecchino, 100 - 45021 Badia Polesine (RO), Italy.


