An implant-supported prosthesis procedure consists in the selection, fabrication, positioning and rehabilitation of one or more missing teeth and their associated structures by means of dental implants. (1) More specifically, the fabrication of a fixed prosthesis on a single-tooth implant is referred to as an implant-supported crown. (1)
In cases where a single tooth is missing, implant-supported crowns are an increasingly popular option for prosthetic rehabilitation. (2)
The replacement of a missing tooth can now be included among the classic indications for the fabrication of a single-implant fixed prosthesis. (3,4) Although certain complications may arise, the literature shows that the long-term (5-10 years) survival rate for this type of prosthesis is high. (5-7)
Conventional clinical procedure
The clinical phases for making fixed prostheses on single implants, be they cement- or screw-retained, can vary depending on the clinical case and the type of prosthetic restoration. (8)
The conventional procedure is described below, without mentioning any alternative techniques.
We will now focus on the conventional clinical phases for fabricating fixed prostheses on single implants.
Surgical uncovering and the healing screw
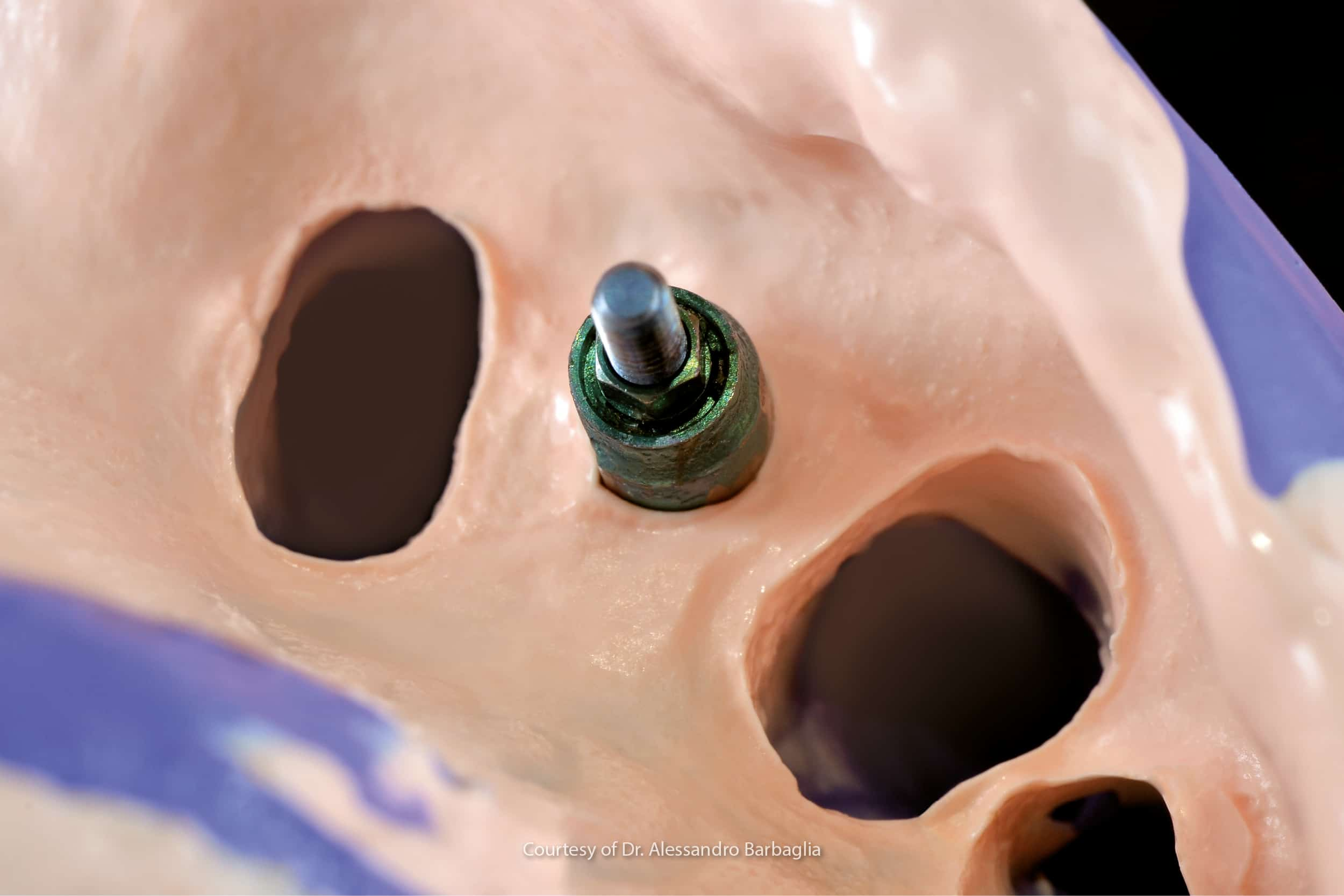
Once the proper osteointegration times have elapsed, considering also the anatomical area involved, it is possible to proceed with the surgical uncovering of the implant emergence.
Once access to the implant emergence has been established, the cap screw protecting the implant connections will be removed and replaced by healing screw with a clinical case-specific diameter and height.
The healing screw guides the healing of the soft tissues in creating a mucosal tunnel between the implant connection and the oral cavity proper, in order to simplify the subsequent prosthetic rehabilitation.
This procedure is not followed when:
- a ‘one-step’ surgical approach is adopted. i.e. when the healing screw is inserted at the same time as the implant is placed (9);
- the placed implant is not “bone level”, i.e. with the head of the implant level with the bone crest, but “tissue level”, i.e. it has a smooth transmucosal collar that allows the tissues to adapt while osteointegration takes place. (10)
It is not until the end of the time required for the complete healing and maturation of the peri-implant tissues, which can be affected by the type of surgery, type of healing screw and amount of keratinised gum (11), that it is possible to proceed with the fundamental impression phase.
Analogue or digital impression phase
This process can be carried out with analogue techniques, using different types of material (including polyvinylsiloxanes and polyethers) and different types of technique (including snap or closed tray impressions and pick-up or open tray impressions). (12,13) Alternatively, when using a digital workflow, it is possible to opt for an intraoral scan. (14)
At the analogue or digital level, the implant analogue is placed at the pick up connection and in continuity with the scan body This makes it possible to obtain a positive model containing the three-dimensional spatial position of the implant. (15)
This is fundamental, as the dental technician will use it to fabricate the future rehabilitation. Consequently, great care must be taken during all the impression phases not to jeopardise the final result.
Want to find out more?
Read the in-depth focus on the comparison between analogue and digital impressions
Depending on the specific clinical case and the type of prosthesis prescribed by the dentist (cement-retained, screw-retained, etc.), intermediate phases may be required before the final prosthesis is delivered.
Some fundamental aspects to check
During the various tests, it is necessary to check multiple aspects that can affect the successful outcome of the rehabilitation therapy:
- proper connection coupling (also by means of a follow-up x-ray) (16);
- the proper occlusal relationship with the antagonist, under conditions of maximum intercuspation during lateral, protrusive and retrusive disclusion movements;
- the adequacy of the interproximal contacts (17,18), which can be checked using dental floss.
Once all these tests have been passed, the crown can be definitively delivered to the patient, who will have regular follow-up appointments.
Hydrorise System is the complete range of Zhermack addition silicones for impression-taking on both implants and natural tooth stumps and was developed for practitioners looking for high-performance solutions.
References
- The Glossary of Prosthodontic Terms: Ninth Edition. J Prosthet Dent 2017;117: e1-e105 n.d.
- Behneke N, Schramm-Scherer B, Behneke G, Schmitz R. Zur Differentialindikation bei Einzelzahnverlust—Einzelzahnspätimplantat oder Adhäsivbrücke. Z Zahnärztl Implantol 1988;4:135–138.
- Alkbretsson T, Dahl E, Enbom L, Engevall S, Engquist B, Eriksson AR, et al. Osseointegrated oral implants. A Swedish multicenter study of 8139 consecutively inserted Nobelpharma implants. J Periodontol 1988;59:287–296.
- Apse P, Zarb GA, Schmitt A, Lewis DW. The longitudinal effectiveness of osseointegrated dental implants. The Toronto study: Peri-implant mucosal response. Int J Periodont Rest Dent 1991;11:95–108.
- Jung, R. E., Pjetursson, B. E., Glauser, R., Zembic, A., Zwahlen, M., & Lang, N. P. (2008). A systematic review of the 5‐year survival and complication rates of implant‐supported single crowns. Clinical oral implants research, 19(2), 119-130.
- Hjalmarsson, L., Gheisarifar, M., & Jemt, T. (2016). A systematic review of survival of single implants as presented in longitudinal studies with a follow-up of at least 10 years. Eur J Oral Implantol, 9(Suppl 1), S155-62.
- Tey, V. H., Phillips, R., & Tan, K. (2017). Five‐year retrospective study on success, survival and incidence of complications of single crowns supported by dental implants. Clinical oral implants research, 28(5), 620-625.
- Lops, D., Bruna, E., & Fabianelli, A. (2014). La protesi implantare. Dental Cadmos, 6(82), 386. n.d.
- Assaf, M., & Alaa’Z, A. G. (2014). Screw-retained crown restorations of single implants: A step-by-step clinical guide. European journal of dentistry, 8(04), 563-570.
- Fernández-Formoso N, Rilo B, Mora MJ, Martínez-Silva I, Díaz-Afonso AM. Radiographic evaluation of marginal bone maintenance around tissue level implant and bone level implant: a randomised controlled trial. A 1-year follow-up. Journal of Oral Rehabilitation 2012;39:830–7. https://doi.org/10.1111/j.1365-2842.2012.02343.x.
- Mattheos, N., Vergoullis, I., Janda, M., & Miseli, A. (2021). The implant supracrestal complex and its significance for long-term successful clinical outcomes. The International journal of prosthodontics, 34(1), 88-100.
- https://magazine.zhermack.com/studio/implantologia-impronta-pick-up-e-impronta-a-strappo/
- Chee, W., & Jivraj, S. (2006). Impression techniques for implant dentistry. British dental journal, 201(7), 429-432.
- Marques, S., Ribeiro, P., Falcão, C., Lemos, B. F., Ríos-Carrasco, B., Ríos-Santos, J. V., & Herrero-Climent, M. (2021). Digital impressions in implant dentistry: A literature review. International journal of environmental research and public health, 18(3), 1020.
- Mühlemann, S., Greter, E. A., Park, J. M., Hämmerle, C. H., & Thoma, D. S. (2018). Precision of digital implant models compared to conventional implant models for posterior single implant crowns: A within‐subject comparison. Clinical oral implants research, 29(9), 931-936.
- Papavassiliou, H., Kourtis, S., Katerelou, J., & Chronopoulos, V. (2010). Radiographical evaluation of the gap at the implant‐abutment interface. Journal of Esthetic and Restorative Dentistry, 22(4), 235-250.
- Boyarsky, H. P., Loos, L. G., & Leknius, C. (1999). Occlusal refinement of mounted casts before crown fabrication to decrease clinical time required to adjust occlusion. The Journal of prosthetic dentistry, 82(5), 591-594.
- Hellsing, G. (1988). Occlusal adjustment and occlusal stability. The Journal of prosthetic dentistry, 59(6), 696-702.
Do you want more information on Zhermack Dental products and solutions?
Contact us

 Zhermack SpA has been one of the most important producers and international distributors of alginates, gypsums and silicone compounds for the dental sector for over 40 years. It has also developed solutions for the industrial and wellbeing sectors.
Zhermack SpA - Via Bovazecchino, 100 - 45021 Badia Polesine (RO), Italy.
Zhermack SpA has been one of the most important producers and international distributors of alginates, gypsums and silicone compounds for the dental sector for over 40 years. It has also developed solutions for the industrial and wellbeing sectors.
Zhermack SpA - Via Bovazecchino, 100 - 45021 Badia Polesine (RO), Italy.


