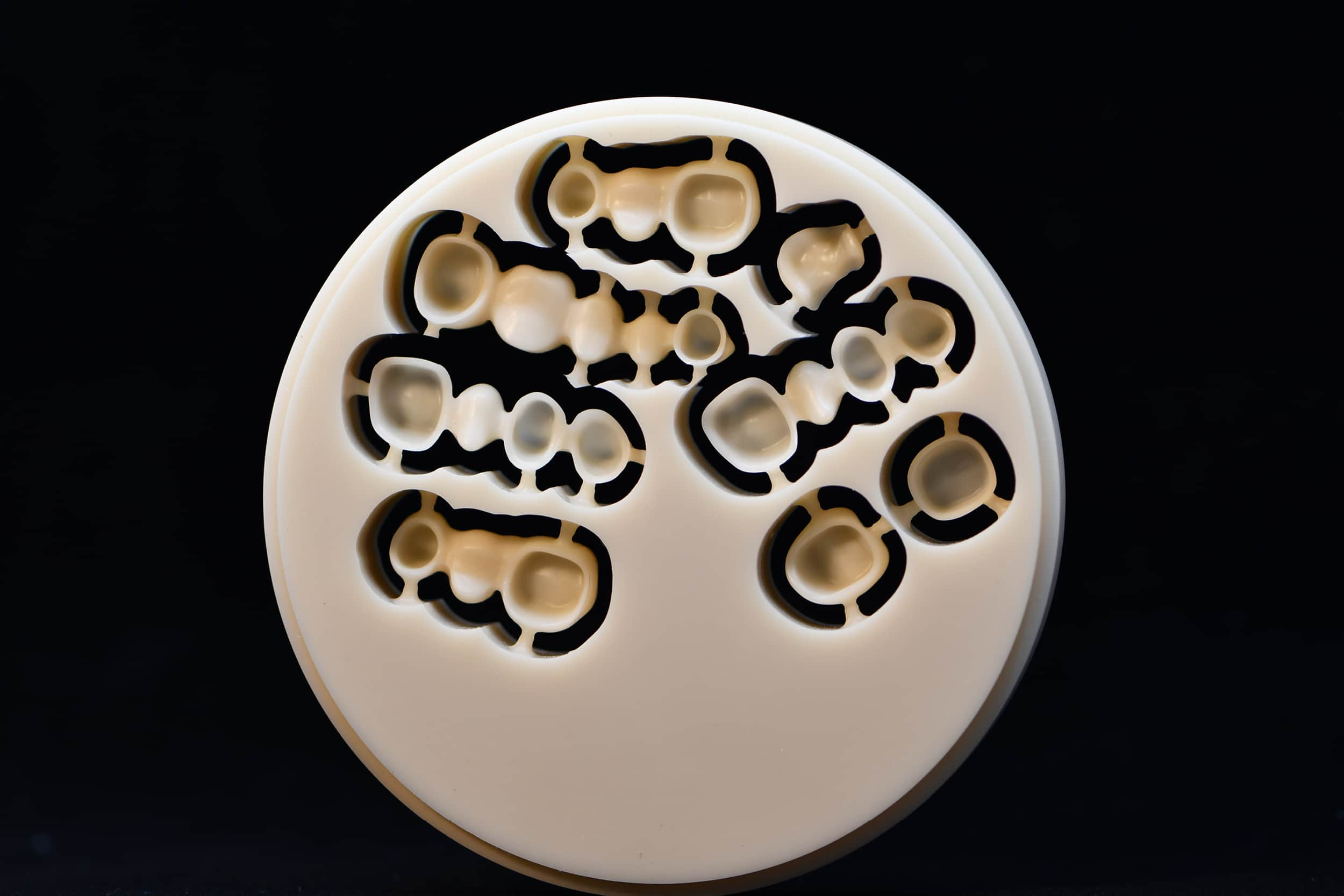
The innovation brought about by digital technologies has now partly or completely revolutionised certain workflows, not only in dental practices, but also in dental laboratories [1–3]. In dental laboratories, digital workflows have accelerated various procedures that in the past, with analogue methods, were very time-consuming for dental technicians (for further information see Digital laboratories and next-generation dental technicians: past vs present).
This came about mainly with the advent of conventional computer numerical control (CNC) milling machines [4,5]. These automatic machines consist of one or more cutting instruments, which move on a certain number of axes and, based on a design created by the dental technician in the CAD (Computer-Aided Design) phase, mill a disk of homogeneous material to obtain a prosthetic restoration [1].
A disk can be used to obtain any type of restoration in terms of size and extent; however, smaller restorations, such as inlays, single crowns and bridges of up to three elements are generally more simply created from blocks [5].
Disks therefore allow technicians to produce extensive restorations of the arches fairly quickly.
Polymethyl methacrylate disks (PMMA)
PMMA (polymethyl methacrylate) disks can now be used to obtain full removable dentures, including both the pink denture body and the dentition, or just one of the two parts, bringing considerable clinical and technical advantages [6,7].
Clinically, denture bases milled from a disk of pre-cured resin are free from cure shrinkage, which is intrinsic to conventionally processed bases (resin curing in a hot or cold flask) [8,9].
This results in better tissue adaptation of milled denture bases, but also in a lower risk of dental movements during or after the curing of the resin in the flask [8,9].
In addition, the overall release of monomer (in the mouth and during the fabrication of the denture) is far lower, while the mechanical strength of the denture is greater, due to the lower porosity of the resin component [10].
The improved biocompatibility properties and, in particular, lower porosity also ensure milled dentures lower adhesion for bacteria and fungi such as Candida albicans and extrinsic pigmentation [10,11].
Teeth milled from disks
As far as teeth milled from disks are concerned, it is important to know that they can be milled individually, in sextants/quadrants or even as whole arches [12]. The disks from which they are milled can be monochromatic or polychromatic, for better aesthetic results, despite not being comparable to conventional multilayer acrylic teeth sold in sets of six [7].
However, as they originate from a block of industrially pre-cured resin, milled teeth offer levels of wear-resistance that are superior even to those of acrylic teeth and certainly far better than 3D-printed teeth [12]. In addition, the shape of the teeth can be chosen and altered as desired, as they are based on a CAD design.
From a financial point of view, considering the entire production chain, including the production of the restoration, clinical chair time and laboratory time, the costs are considerably lower with the milled denture protocol than with the conventional protocol, although the material expenses are higher [6].
Modified PMMA disks
Disks can also be used to mill provisional devices not only in conventional PMMA, but also with modified PMMA, in order to improve certain characteristics such as fracture resistance or oral cavity longevity [13,14].
In this regard, long-term provisional devices may benefit from these new materials, which are now available thanks to the subtractive techniques of digital restoration production.
Furthermore, subtractive techniques that make it possible to mill any type of material have paved the way also for the use of polymeric materials that were previously unheard of or never used in dentistry, such as polyether ether ketone or PEEK.
PEEK is a highly-ordered, flexible, strong, shape-stable, biocompatible technopolymer that provides a useful framework for partial dentures and implant-based restorations [15,16].
However, its mechanical, aesthetic and biocompatibility characteristics have yet to be tested over the long term in order to be able to define it a material for permanent restorations [17].
Conclusions
It can therefore be concluded that thanks to disks and, more generally, subtractive production techniques, resin materials generally afford better mechanical properties than their conventional counterparts [18,19] and have also made it possible to explore further opportunities provided by the new polymers within a fairly short period [17].
Nevertheless, it should be pointed out that even these systems do not make it possible to fabricate permanent restorations with the aesthetic properties required for direct application in the oral cavity and they in any case require aesthetic characterisation (pigmentation, glazing, application of the seal coat) by the dental technician before being sent to the clinician.
Lastly, there are still many new polymeric materials suitable for milling to be studied in the long term.
References
[1] Masri R, Driscoll C. Odontoiatria digitale: Presupposti teorici e applicazioni cliniche. Edra; 2017.
[2] Maragliano-Muniz P, Kukucka ED. Incorporating Digital Dentures into Clinical Practice: Flexible Workflows and Improved Clinical Outcomes. J Prosthodont 2021;30:125–32. https://doi.org/10.1111/jopr.13277.
[3] Seelbach P, Brueckel C, Wöstmann B. Accuracy of digital and conventional impression techniques and workflow. Clin Oral Investig 2013;17:1759–64. https://doi.org/10.1007/s00784-012-0864-4.
[4] Lebon N, Tapie L, Duret F, Attal J-P. Understanding dental CAD/CAM for restorations – dental milling machines from a mechanical engineering viewpoint. Part A: chairside milling machines. Int J Comput Dent 2016;19:45–62.
[5] N L, L T, F D, Jp A. Understanding dental CAD/CAM for restorations–dental milling machines from a mechanical engineering viewpoint. Part B: labside milling machines. International Journal of Computerized Dentistry 2016;19.
[6] Srinivasan M, Schimmel M, Naharro M, O’ Neill C, McKenna G, Müller F. CAD/CAM milled removable complete dentures: time and cost estimation study. Journal of Dentistry 2019;80:75–9. https://doi.org/10.1016/j.jdent.2018.09.003.
[7] Srinivasan M, Kamnoedboon P, McKenna G, Angst L, Schimmel M, Özcan M, et al. CAD-CAM removable complete dentures: A systematic review and meta-analysis of trueness of fit, biocompatibility, mechanical properties, surface characteristics, color stability, time-cost analysis, clinical and patient-reported outcomes. J Dent 2021;113:103777. https://doi.org/10.1016/j.jdent.2021.103777.
[8] Goodacre CJ, Goodacre BJ, Baba NZ. Should Digital Complete Dentures Be Part of A Contemporary Prosthodontic Education? J Prosthodont 2021;30:163–9. https://doi.org/10.1111/jopr.13289.
[9] Hwang H-J, Lee SJ, Park E-J, Yoon H-I. Assessment of the trueness and tissue surface adaptation of CAD-CAM maxillary denture bases manufactured using digital light processing. J Prosthet Dent 2019;121:110–7. https://doi.org/10.1016/j.prosdent.2018.02.018.
[10] Steinmassl O, Offermanns V, Stöckl W, Dumfahrt H, Grunert I, Steinmassl P-A. In Vitro Analysis of the Fracture Resistance of CAD/CAM Denture Base Resins. Materials (Basel) 2018;11:401. https://doi.org/10.3390/ma11030401.
[11] Al-Fouzan AF, Al-Mejrad LA, Albarrag AM. Adherence of Candida to complete denture surfaces in vitro: A comparison of conventional and CAD/CAM complete dentures. J Adv Prosthodont 2017;9:402–8. https://doi.org/10.4047/jap.2017.9.5.402.
[12] Silva NRFA, Kukucka ED. Innovative subtractive production of a digital removable complete denture from start to finish: a JPD Digital video presentation. The Journal of Prosthetic Dentistry 2022;127:1–5. https://doi.org/10.1016/j.prosdent.2021.12.002.
[13] Ionescu AC, Brambilla E, Pires PM, López-Castellano A, Alambiaga-Caravaca AM, Lenardi C, et al. Physical-chemical and microbiological performances of graphene-doped PMMA for CAD/CAM applications before and after accelerated aging protocols. Dent Mater 2022;38:1470–81. https://doi.org/10.1016/j.dental.2022.06.032.
[14] Selva-Otaolaurruchi EJ, Fernández-Estevan L, Solá-Ruiz MF, García-Sala-Bonmati F, Selva-Ribera I, Agustín-Panadero R. Graphene-Doped Polymethyl Methacrylate (PMMA) as a New Restorative Material in Implant-Prosthetics: In Vitro Analysis of Resistance to Mechanical Fatigue. J Clin Med 2023;12:1269. https://doi.org/10.3390/jcm12041269.
[15] The Glossary of Prosthodontic Terms. The Journal of Prosthetic Dentistry 2017;117:C1-e105. https://doi.org/10.1016/j.prosdent.2016.12.001.
[16] Piscopo M, Grande F, Catapano S. Full Digital Workflow for Prosthetic Full-Arch Immediate Loading Rehabilitation Using OT-Bridge System: A Case Report. Prosthesis 2022;4:213–23. https://doi.org/10.3390/prosthesis4020021.
[17] Blanch-Martínez N, Arias-Herrera S, Martínez-González A. Behavior of polyether-ether-ketone (PEEK) in prostheses on dental implants. A review. J Clin Exp Dent 2021;13:e520–6. https://doi.org/10.4317/jced.58102.
[18] Alghazzawi TF. Advancements in CAD/CAM technology: Options for practical implementation. Journal of Prosthodontic Research 2016;60:72–84. https://doi.org/10.1016/j.jpor.2016.01.003.
[19] Grande F, Mochi Zamperoli E, Pozzan MC, Tesini F, Catapano S. Qualitative Evaluation of the Effects of Professional Oral Hygiene Instruments on Prosthetic Ceramic Surfaces. Materials 2021;15:21. https://doi.org/10.3390/ma15010021.
Do you want more information on Zhermack Dental products and solutions?
Contact us


 Zhermack SpA has been one of the most important producers and international distributors of alginates, gypsums and silicone compounds for the dental sector for over 40 years. It has also developed solutions for the industrial and wellbeing sectors.
Zhermack SpA - Via Bovazecchino, 100 - 45021 Badia Polesine (RO), Italy.
Zhermack SpA has been one of the most important producers and international distributors of alginates, gypsums and silicone compounds for the dental sector for over 40 years. It has also developed solutions for the industrial and wellbeing sectors.
Zhermack SpA - Via Bovazecchino, 100 - 45021 Badia Polesine (RO), Italy.


